Mwansuda had an excruciating pregnancy. The threshold for severe anaemia in pregnant women is 70 grams of haemoglobin per litre of blood. Mwansuda bled so much during pregnancy that her haemoglobin fell to 60 g/L. An ultrasound revealed that one of her two foetuses had died. “I cried so much because I had hoped to carry twins”, said Mwansuda.
When Naramatisho entered the delivery room her haemoglobin was 27 g/L. She hadn’t needed to be told that her baby was dead. “I knew my baby was no more”, said Naramatisho. “She wasn’t kicking…she was no longer playful, until she was totally quiet”. Naramatisho still had to go through with the birth, though. She delivered her dead baby and then lost consciousness. It took a blood transfusion to revive her. She has nothing but praise for the staff: “these doctors did a good job”.
It is almost inconceivable that a woman in the UK would give birth with haemoglobin as low as Naramatisho’s
“It would be a medical emergency. The obstetrician is not going to let it get to that stage – they would take action much earlier in the pregnancy”, explained Haleema Shakur-Still, Emeritus Professor of Global Health Clinical Trials at the London School of Hygiene & Tropical Medicine (LSHTM). But Mwansuda and Naramatisho were not in the UK. They were in Tanzania.
Postpartum haemorrhage (PPH), which WHO now defines as blood loss amounting to 300 ml or more within 24 hours of birth, affects 14 million women around the world every year. But the vast majority of the 70,000 deaths or so from the condition occur in sub-Saharan Africa and South Asia, where tens of millions of women have anaemia. “Anaemia is so common in these regions that people do not pay any attention”, said Shakur-Still. “They do not think it is such a big deal if you give birth with extremely low levels of haemoglobin”. But it most certainly is a big deal.

A woman lies in a hospital bed while two other women examine her stomach
Shakur-Still co-led the WOMAN-2 study, which recruited more than 15,000 pregnant women with anaemia across Nigeria, Tanzania, Zambia and Pakistan. It found that women with severe anaemia were seven times more likely to die from PPH than women with moderate anaemia. If haemoglobin falls to 50 g/L, the risk of PPH rises to 20% and the risk of stillbirth reaches an astonishing 32%.
The findings from the WOMAN-2 Trial are outlined in a new report from LSHTM and team of global collaborators, The missing evidence: anaemia, postpartum bleeding and maternal death. It makes for stark reading. “The WOMAN-2 data demand an urgent reappraisal of global PPH policy. It is anaemia that is killing mothers”, write the authors, who include Shakur-Still. They issue a call to arms: “Advocacy and decisive action to cut the prevalence and severity of anaemia in women and adolescent girls is urgently needed to reduce maternal deaths”.
For women with severe anaemia, even a small amount of blood loss during childbirth can be catastrophic. Dr Ian Roberts is Professor of Epidemiology and Public Health at LSHTM and co-lead of the WOMAN-2 Trial. “The really dangerous thing is shock”, he explained. “That’s when the tissues do not get enough oxygen. If a woman is giving birth and loses a lot of blood, her blood pressure falls, the tissues are starved of oxygen, and she goes into shock. Now she is at risk of organ failure”. Women with severe anaemia are already struggling to supply their tissues with oxygen, since they don’t have enough of the red blood cells that carry oxygen around the body. It does not take much bleeding at all for them to go into shock.
“Say a woman in Canada with a haemoglobin of 130 g/L gives birth”, said Roberts. “She can afford to lose a litre of blood. Her heart rate might rise a little, but she is basically fine. There is plenty of oxygen getting to her tissues. Now imagine a woman in Cameroon, with a haemoglobin of 30 g/L. Even a small loss of blood can put her on the doorstep of death”. WHO has acknowledged that the diagnostic criteria for PPH is inadequate for women with anaemia. But there is still no consensus on a more suitable definition of PPH.
The latest analysis from the results of the WOMAN-2 Trial has highlighted an additional risk factor for PPH: episiotomy. The researchers found that an episiotomy, which involves making a deep scissor cut to the vagina on the assumption that it will help with delivering the baby, almost doubled the chances of PPH in women with anaemia. Among first-time mothers recruited for the WOMAN-2 Trial, rates of episiotomy in Pakistan and Nigeria stood at 81% and 63%, respectively, despite WHO’s recommending against routine use of the procedure.
Professor Rizwana Chaudhri, consultant gynaecologist and obstetrician and lead investigator for the WOMAN-2 Trial in Pakistan, suggested that the fear of a tear could be driving the steep rates of episiotomy in Pakistan. “If there is a simple tear, it is not a big deal. But if the tear extends into the anal sphincter, then it becomes a huge problem. I think because of the fear of the tear, we have still not given up on episiotomies, even though most of the rest of the world has”, she said.
20-year-old Eilima features in one of a series of short videos on anaemia released by LSHTM (the series also features Mwansuda and Naramatisho). She was left in such agony by her episiotomy and blood loss that her interview had to be suspended. She looks shell-shocked as she recounts the circumstances of her pregnancy.
Nike Bello is Professor of Obstetrics and Gynaecology at the University of Ibadan in Nigeria and country lead for the WOMAN-2 Trial. She noted that for millions of women in the global south, pregnancy and childbirth is a traumatic and bewildering experience. “Other than in the big hospitals, childbirth in Nigeria is mostly without anaesthesia”, said Bello. “We do not have epidurals for the average delivery or any other form of pain relief. We expect women simply to breathe it out. Even an uneventful birth is painful, stressful and anxiety ridden. You have someone shouting at you that if you do not push now, you are going to kill your baby, that kind of thing”.
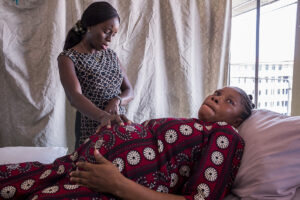
Dr Nike times the contraction of a woman to be sure that it is frequent and strong enough before she sends the patient to the labor ward.
Nigeria does not have universal health coverage. “There is the worry about money, the worry about getting everything you need. Out of the blue, someone mentions anaemia, which you have never heard of before. They tell you how it could affect you, your baby, and the birth – as if things are not already scary enough”, said Bello.
In many low-income settings, access to haemoglobin testing is scarce, so even if anaemia is suspected, confirmation is a challenge. Tranexamic acid is an inexpensive drug which reduces the risk of death from PPH by a third when given within three hours of childbirth. Yet it is not available in every hospital where women give birth. “Tranexamic acid saves lives”, said Roberts. “It is the only drug to have been shown to reduce bleeding deaths in clinical trials. But in the places where it is most needed, it is often not to be found”.
The WOMAN-2 Trial team have come up with a prognostic model to identify women at high risk of life-threatening bleeding. The model is based on data from randomised trials involving more than 45,000 women. It worked well in low-income and middle-income countries and could help clinicians decide whether to prescribe tranexamic acid. “A diagnostic model would be great”, said Shakur-Still, one of the authors of the paper. But she added that it would be preferable to prevent and treat the anaemia long before a woman conceives. “For me, the problem is that anaemia is not being given the priority it warrants”, said Shakur-Still.
Roberts agrees. “It is almost like obstetricians do not even take anaemia into account”, he said. One of the key findings of the WOMAN-2 Trial was that severe anaemia almost doubled the risk of PPH, compared with moderate anaemia. Yet anaemia was not cited as a cause of PPH on the medical records of any of the 742 women who were diagnosed with the condition.
The WOMAN-3 Trial will now examine whether giving tranexamic acid to women during menstruation can help to reduce anaemia. The I’M WOMAN Trial will assess the effects of giving intramuscular or intravenous tranexamic acid just before birth to women at increased risk of postpartum haemorrhage (it is easier to administer tranexamic acid intramuscularly, but it is still unclear whether this is as effective as doing so intravenously).

Blood being arranged for transfusion for Nosheela as she suffers from severe postpartum haemorrhaging at Holy Family Hospital on March 12, 2019 in Rawalpindi, Pakistan. Saiyna Bashir © Wellcome Trust
Since 2016, there has been no meaningful progress in reducing global rates of anaemia or maternal mortality. Roberts pointed out that the WOMAN-2 Trial has categorically shown that women with severe anaemia are at a much greater risk of serious consequences, including death, during childbirth than even women with moderate anaemia. “Anaemia sits in the department of nutrition at WHO. There is a separate department that oversees PPH and anaemia is just not on its radar”, he said. “That means that women are going to continue live with the consequences of anaemia and to die needlessly in childbirth. It is a scandal”.
Bello and Chaudhri, as well as other collaborators on the WOMAN-2 Trial, are working hard on disseminating the findings on anaemia in their home countries. “My colleagues have been open to listening to the new evidence and changing things”, said Bello. “It is a huge task, but we are up for it”, added Chaudhri. “We are going to social media and showing our results to heads of hospital departments”.
“In Pakistan, the poor do not have enough to eat. Even if they are getting enough iron, safe drinking water is in short supply and hookworm infestation is very common, so they become anaemic anyway”, continued Chaudhri. The issue is further complicated by the taboo around menstruation, which is common in many countries around the world, and by some cultural beliefs. “People welcome heavy periods – they think it is a sign of fertility”, said Chaudhri. Moreover, pregnant women often find that the medication for anaemia makes them feel sick (Eilima discontinued treatment for this reason).
Overcoming such a range of challenges is no small task. But that is no reason not to try. Getting the word out about anaemia would be an excellent start. “Last time we were in Nigeria, we spoke to midwives, we spoke to health visitors, we spoke to women, and we discovered that the term ‘anaemia’ does not mean anything to them”, said Roberts. “Everybody needs to know what anaemia is and the kind of consequences it can have. The best way to stop women with anaemia from dying in childbirth is to stop women from going into childbirth with anaemia in the first place”.
Additional Information
Professor Ian Roberts: “According to the WHO, most PPH happens because of the failure of the uterus to contract, something called uterine atony. As a consequence, WHO has based its strategy for reducing PPH on uterotonics, a class of drugs that work by constricting the uterus.
“However, we do not have a single randomised trial showing that uterotonics have any effect on maternal mortality. Women in low-income and middle-income countries mostly go into childbirth without the obstetrician knowing their haemoglobin. When they start bleeding, the obstetrician diagnoses uterine atony and that the solution is uterotonics. Uterine tone is not even measured; it is just assumed to be the problem. Anaemia is not in the conversation. We have taught a generation of obstetricians that it all comes down to the uterus, which is to say, ‘it is the woman’s fault, her body is failing to do what it should be doing’.
“The only drug proven in clinical trials to reduce deaths from bleeding in clinical trials is tranexamic acid, which is recommended by WHO. But the organisation’s response to PPH centres on uterotonics. We have huge global campaigns to increase access to uterotonics because WHO claims they are lifesaving. It is not just that there is no evidence of this – there is not even any evidence that uterotonics do more good than harm. We do have evidence that severe anaemia threatens the lives of women going into childbirth. That is where our focus needs to be.”